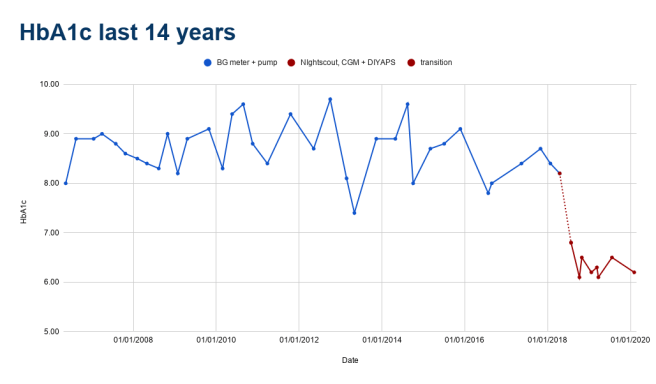
Reading through the latest COVID-19 diabetes statistics from the UK/NHS , I’m reminded that I’m in a much stronger position today with my blood glucose levels than I was two years ago.
Thanks to DIYAPS.
I’m not about to kid myself that I’m invincible – far from it – But it’s sobering to realise that if I do get COVID-19, I’ve got a better chance of not dying from it than I would have, had my blood sugar levels remained the same as they were two years ago.
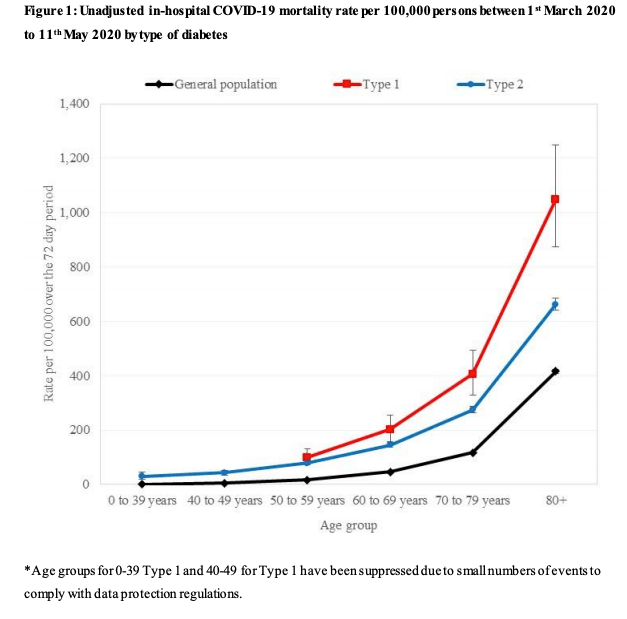
Reflecting on the breakdown of COVID-19 mortality by age in type 1 diabetes, I realise a lot of those in the older age groups that are dying at a greater rate from COVID-19, spent the first decade or two of their diabetes without access to blood glucose monitoring. They relied on urine testing. Compared with BG monitoring it was a blunt tool.
I can remember how blunt a tool it was because a Clinitest tablet in a test tube of urine is what I used to measure my glucose for my first year with type 1 diabetes in 1980. It was part of my therapy, along with one shot a day of long acting insulin.
Apparently my paediatrician loaned us a BG meter for a month when I was thirteen. I asked my mother how the data from this loan period was used. “The doctor told us your blood sugar was high,” she said. I guess he increased my daily dose of insulin when I went to see him at the end of the loan month.
There was a bit of resistance to the idea of patients having their own meters back then. “What would they do with the information?” was a question that was often asked, and some worried about the danger inherent in allowing patients to make their own treatment decisions.
Blood glucose monitoring had a major impact on long term outcomes for people with type 1 diabetes. And this impact can be seen now in the NHS stats.
There’s so much luck in when you were born, where you were born and what resources you have access to.
The latest data is a reminder that diabetes is a generational, historical phenomenon. And that the current moment is ripe with possibilities.
Closed loop systems for type 1 diabetes should make long term side effects of diabetes pretty much negligible. For closed loop people need access to affordable insulin, loopable pumps and CGM.
The solution is actually right here, now. It just needs funding.
Let’s speed the process up. Let’s close the gap in those graph lines.
People with diabetes deserve a healthy future.